What Are Varicose Veins? Unraveling the Mystery
The Anatomy of Varicose Veins: Why Do They Form?
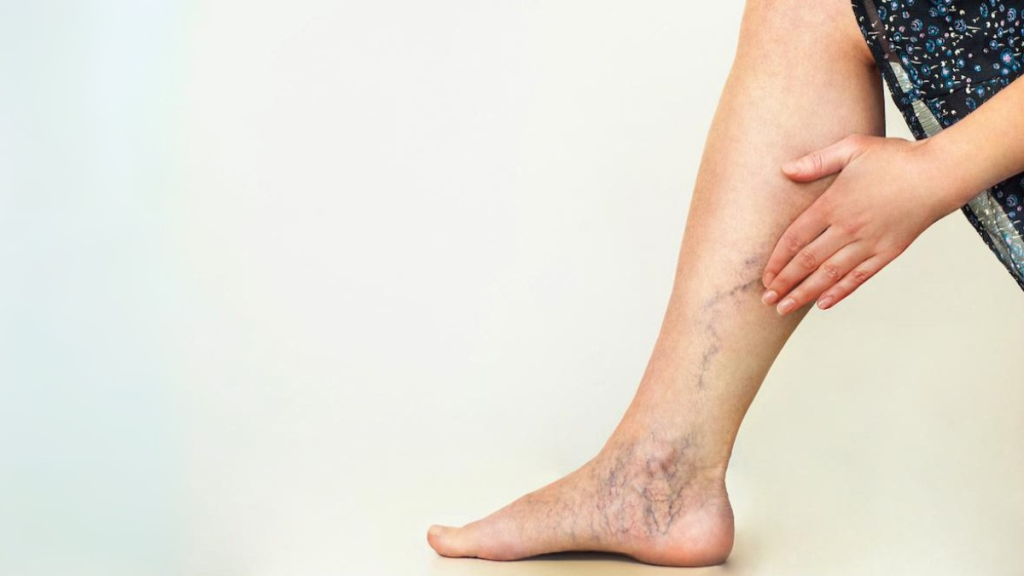
Varicose veins are a common vascular condition characterized by swollen, twisted veins that are visible just under the surface of the skin. They often develop in the legs due to increased pressure in the veins, leading to a malfunction of the venous system. The veins in our legs contain one-way valves that facilitate the upward flow of blood toward the heart. When these valves become weak or damaged, blood can flow backward and pool in the veins, causing them to become enlarged and bulging. This condition is often exacerbated by prolonged periods of standing or sitting, which increases pressure in the leg veins. Additionally, varicose veins can be a result of hereditary factors, hormonal changes such as those experienced during pregnancy, menopause, or with the use of birth control pills, and age-related changes in vein elasticity.
Common Symptoms: How to Recognize Varicose Veins
Recognizing varicose veins involves identifying a range of symptoms that may accompany the visual signs of the condition. The primary symptom is, of course, the appearance of the twisted, bulging veins, typically found on the legs. However, sufferers may also experience a variety of other symptoms including aching, heavy legs, swelling, and cramps, particularly after prolonged periods of sitting or standing. Additionally, itching, skin discoloration, and the development of sores or ulcers around the ankle region can signal severe varicose veins and require medical evaluation. The discomfort caused by varicose veins can significantly affect daily life, leading individuals to avoid certain activities or wear clothing that conceals their legs, which can impact self-esteem and overall quality of life.
Risk Factors: Are You Prone to Varicose Veins?
Understanding the risk factors associated with varicose veins can help individuals identify their likelihood of developing this condition. Age is a significant factor, as the elasticity of veins tends to decrease with age, making valve failure more probable. Gender also plays a role; studies indicate that women are more likely than men to develop varicose veins, largely due to hormonal influences. Genetic predisposition is another factor, as having a family history of varicose veins increases one’s risk. Other lifestyle aspects contributing to this condition include obesity—excess weight adds pressure on leg veins—and sedentary lifestyles that do not promote healthy circulation. Pregnant women experience temporary changes in hormone levels and blood volume, making them more prone to varicose veins during and shortly after pregnancy. Ultimately, identifying these risk factors is crucial for prevention efforts and early intervention.
Cutting-Edge Treatments: A Look at Varicose Vein Removal Options
Non-Invasive Solutions: Sclerotherapy and Beyond
Sclerotherapy is one of the most popular non-invasive treatments for varicose veins. This procedure involves injecting a sclerosing agent directly into the vein, which irritates the vein’s lining, causing it to collapse and eventually fade from view. This method is particularly effective for smaller varicose veins and spider veins. Most patients report minimal discomfort during the procedure, often resembling a slight pinprick. Sclerotherapy is typically performed in the doctor’s office and does not require anesthesia, allowing individuals to return to their daily activities shortly after treatment. Alongside sclerotherapy, other non-invasive options such as compression therapy can support vein health by improving circulation and minimizing discomfort.
Laser Treatments: The Future of Vein Removal
Advancements in medical technology have led to the development of laser treatments for varicose veins, representing a non-surgical alternative to traditional vein removal. Laser therapy works by targeted application of light energy, which heats the vein tissues, causing them to collapse and seal shut. Endovenous laser therapy (EVLT) has become particularly popular due to its minimally invasive nature and effective results. Patients undergoing laser treatment often experience less discomfort and a shorter recovery time compared to traditional surgical methods. Another innovative technique is the use of intense pulsed light therapy (IPL), which aids in reducing the appearance of superficial veins. Both laser treatments continue to gain favor, as they are associated with lower complication rates and quicker return to regular activities.
Traditional Surgery: When Is It Necessary?
In cases where varicose veins cause significant pain, swelling, or complications such as ulcers or blood clots, traditional surgical intervention may be warranted. Surgical options primarily include vein stripping, where the affected vein is surgically removed through small incisions. While this procedure can be very effective in alleviating symptoms and improving appearance, it is usually recommended for extensive varicose veins or those that have not responded to other treatments. Patients often require local or general anesthesia, and recovery time can be longer, involving several weeks before full mobility returns. Nevertheless, traditional surgical methods remain relevant, particularly for severe cases where less invasive treatments are insufficient.
Preparing for Your Procedure: What You Need to Know
Consultations and Assessments: Setting Realistic Expectations
Before undergoing any varicose vein treatment, it’s vital to schedule a detailed consultation with a qualified healthcare provider. During the assessment, the provider will conduct a thorough examination of your legs, review your medical history, and may recommend an ultrasound study to examine the blood flow in your veins. This evaluation is crucial for determining the most suitable treatment approach tailored to your specific situation. Open communication about your symptoms, concerns, and desired outcomes is paramount. Setting realistic expectations regarding the results, treatment duration, and recovery time will facilitate a smoother process. Additionally, discussing potential risks and side effects of the proposed treatment allows you to make an informed decision.
What to Do Before Your Appointment: Tips for Success
Preparation for your appointment can greatly influence the effectiveness of your treatment. It is advisable to wear loose-fitting clothing on the day of the consultation to allow easy examination of your legs. Document any medications, vitamins, and herbal supplements you are currently taking, as these can affect treatment choices. Ensure you relay any allergies or prior adverse reactions to anesthesia or medications to your provider. If you are a smoker, consider quitting or reducing your intake, as smoking can impair circulation and negatively impact healing. Lastly, familiarize yourself with post-procedure care tips, which will be essential after treatment.
Post-Procedure Care: Ensuring a Smooth Recovery
Post-procedure care is integral to achieving optimal results from your varicose vein treatment. Immediately following the procedure, patients are often advised to wear compression stockings to enhance blood flow and support the healing process. Gentle walking is encouraged shortly after the treatment to promote circulation; however, high-impact activities and heavy lifting should be avoided for several days. It’s important to monitor your legs for any complications such as increased pain, swelling, or signs of infection as these can necessitate further medical attention. Attending follow-up appointments will allow your healthcare provider to monitor your recovery and address any concerns.
Living Legally: Embracing a Healthier Lifestyle Post-Treatment
Long-Term Care: Maintaining Healthy Veins After Removal
Once you’ve undergone varicose vein removal, maintaining your vein health becomes essential to prevent recurrences and ensure long-lasting results. Regular follow-up appointments with your healthcare provider will help monitor your condition and allow for any necessary interventions. Incorporating habits like wearing compression stockings during prolonged sitting or standing can enhance circulation and support your veins. Staying hydrated is also vital, as proper hydration aids in maintaining healthy blood flow. Integrating elements of vein care into daily routines can significantly contribute to your overall wellness.
Exercise and Diet: Best Practices for Vein Health
Engaging in regular exercise plays a crucial role in promoting healthy veins and minimizing the risk of developing new varicose veins. Low-impact exercises, such as walking, cycling, and swimming, encourage blood circulation without overstraining the veins. Activities that focus on leg elevation, like yoga or stretching, can help alleviate pressure in the veins and optimize circulation. Coupled with exercise, adopting a balanced diet rich in fiber, antioxidants, and anti-inflammatory foods can support vascular health. Foods such as leafy greens, berries, nuts, and whole grains can promote healthy blood flow and protect the vascular system.
Monitoring Your Legs: When to Seek Professional Advice
Being proactive in monitoring the condition of your legs post-treatment is essential for ensuring long-term vein health. People should remain vigilant for signs of new varicose veins or complications that may arise post-procedure. Symptoms such as persistent swelling, unexpected pain, or changes in skin color should prompt immediate consultation with a healthcare provider. Don’t hesitate to reach out if you notice any unusual changes or have concerns, as early intervention can prevent more serious complications and maintain overall leg health. Being attentive to your body can ensure that you enjoy the benefits of your varicose vein treatment for years to come.